Strathclyde People 2017
Ask people of a certain age to think about biomedical engineering and the conversation inevitably turns to Steve Austin – television’s bionic man and star of 1970s television show The Six Million Dollar Man.
Surprisingly, it’s not an analogy that completely offends Professor Terry Gourlay. As Head of the Department of Biomedical Engineering at Strathclyde, he oversees the application of technology and engineering to surgery and medicine.
“I hear this a lot,” he said patiently, “but the truth is, we are still dealing with the components. Joining them together to produce a Steve Austin is still far over the horizon technically and financially.”
Even if the department is not about to create a man of superhuman strength anytime soon, the reality is even more compelling.
Within a collaborative research environment, staff and students are finding amazing engineering solutions to today’s global healthcare challenges. Specific areas of research include medical devices and diagnostics; rehabilitation engineering; and cell, tissue and organ engineering.
“Our goal is to transform and improve future healthcare through innovations and advances in science and technology,” said Professor Gourlay. “We focus on the clinical problems of today to improve the healthcare of tomorrow.”
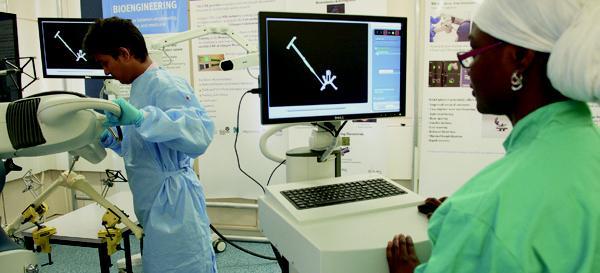
The intelligent robotic drill was developed at the department for Biomedical Engineering
Thanks to biomedical engineering research at the University, several remarkable medical devices are now making the transition from laboratory bench to real-life situations. For example, Professor Gourlay’s research group have developed blood salvage technology, which is transforming the way surgery is carried out.
The device, called HemoSep, is designed to recover blood during open-heart and major trauma surgery, and concentrate the cells for transfusion back to the patient. In clinical trials, HemoSep significantly reduced the need for blood transfusion and the problems associated with transfusion reactions.
In another sector of medical practice, the WoundSense™ moisture sensor was developed by Ohmedics Ltd – a company set up by the department’s bioengineers – and allows doctors and nurses to check the status of a wound without removing the dressing.
Other technological developments include a portable eye examination kit which is helping to increase access to eye care worldwide and a paediatric ECMO, an artificial heart and lungs for children that’s used instead of conventional cardiopulmonary bypass systems.
It is perhaps no surprise that the founders of the department in 1963 were a plastic surgeon and a civil engineer. Tom Gibson and Robert Kenedi not only established the first bioengineering unit in Europe, they also started an enduring relationship between healthcare and engineering at the University that remains as innovative today as it is practical.
“We don’t want what we do to be the stuff of science fiction,” said Professor Bernard Conway, who leads the department’s research in rehabilitation engineering. “It needs to translate into everyday life, and contribute to the welfare and wellbeing of people needing help.“That’s why interacting with hospitals and clinics is essential.”
Rehabilitation engineering needs to translate into everyday life, and contribute to the welfare and wellbeing of people needing help.”
Professor Bernard Conway
While colleagues have developed an intelligent drill and navigation system for orthopaedic surgery that will significantly improve implant positioning and patient outcomes, others have close relationships with the Queen Elizabeth National Spinal Injuries Unit at Glasgow’s Queen Elizabeth University Hospital and stroke units throughout the city.
Here, University staff are seeking to understand more about people’s recovery mechanisms in order to improve rehabilitation outcomes from stroke or spinal cord trauma. For example, Dr Andy Kerr, a specialist in physiotherapy and stroke rehab, is working with advanced robotics to create ‘virtual’ assistants that reduce the need for one-to-one physiotherapy.
Others have developed ‘robotic clothes’ to help people with mobility problems move easily and unaided, and live more independent lives.
While the cutting-edge of prosthetics research includes ‘bionic’ limbs that can be controlled by brain activity, the department also faces more practical challenges – such as helping to meet the high demand for high-quality but affordable artificial limbs in developing countries.
In response, Dr Arjan Buis, a senior research fellow who has received funding from Google, leads a team that has developed sockets, known as Majicast, which fit prostheses securely to patients’ residual limbs.
Meanwhile, Professor Helen Grant and colleagues are leading a research stream that explore the way the body’s cells interact with the materials used in implants.
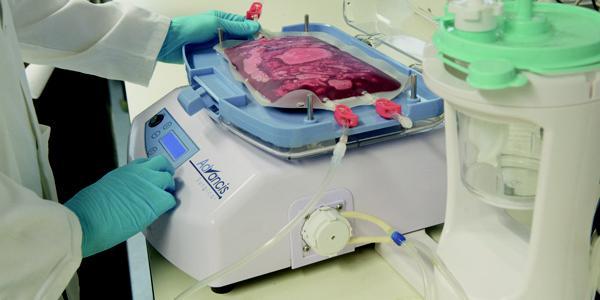
HemoSep recovers blood during major trauma surgery and concentrate the cells for transfusion
back to the patient
Most recently, the department has appointed Professor Will Shu as the Hay Chair in Paediatric Health, thanks to the support of a senior alumnus. Professor Shu is pioneering the use of 3D printing to produce printed tissues. This technology has the potential to replace artificial materials in implantable devices, enhancing durability and reducing the likelihood of rejection.
It may be technology unimagined by Gibson and Kenedi back in 1963 but the need for financial support would be very familiar – it was an initial grant from the Medical Research Council that helped the founders establish the department.
Since then, the visionary support of the Wolfson Foundation saw the construction of the Wolfson Centre as the department’s hub in 1974. Today, philanthropic support continues to make a significant difference to Biomedical Engineering at Strathclyde.
Funding has enabled the development of world-class technology and staff – but now the support of alumni is required more than ever as the department faces one of its biggest challenges.
Although the Wolfson Centre has served staff and students well, it now needs to be completely redeveloped to enable the department to enhance its global reputation as a biomedical engineering research centre.

Virtual motion analysis at the department of Biomedical Engineering
Following a grant of £750,000 towards the redevelopment from the Wolfson Foundation in June 2017, the University is now engaged in raising a further £2.25 million towards the total cost of £15.1 million.
This investment will create new labs and refurbish existing facilities, encourage greater collaboration with industry and the NHS, offer more undergraduate and postgraduate places, and train a new generation of innovative biomedical engineers.
“With this support, we will be able to continue offering prospective partners, students and visiting researchers a world-class environment that facilitates original thinking and delivers research that has a positive impact on clinical care and quality of life,” added Professor Gourlay.
The £15 million redevelopment of the Wolfson Centre for Biomedical Engineering will invest in this leading centre for medical technologies, clinical solutions and the education of world-class biomedical engineers. To find out how you can help solve today’s clinical problems to transform the healthcare of tomorrow, please email alumni@strath.ac.uk










